The Diabetes and Neuropathy Relationship: A 2026 Survival Guide
“High blood sugar doesn’t just sit in the veins; it systematically dismantles the communication lines between your brain and your body.”
The diabetes and neuropathy relationship is arguably the most critical intersection in modern metabolic health. For decades, we viewed nerve damage as an inevitable “side effect,” but in 2026, we understand it as a direct biological consequence of glucose-induced oxidative stress. According to the American Diabetes Association, nearly half of all diabetic patients will face some form of neuropathy, making early intervention not just an option, but a necessity.
The “Sandpaper” Effect:
Think of high glucose levels as invisible “sandpaper” on your nerves. It wears down the protective myelin sheath—the insulation that allows electrical signals to travel—and starves the nerve of the oxygen-rich blood it needs to stay alive.
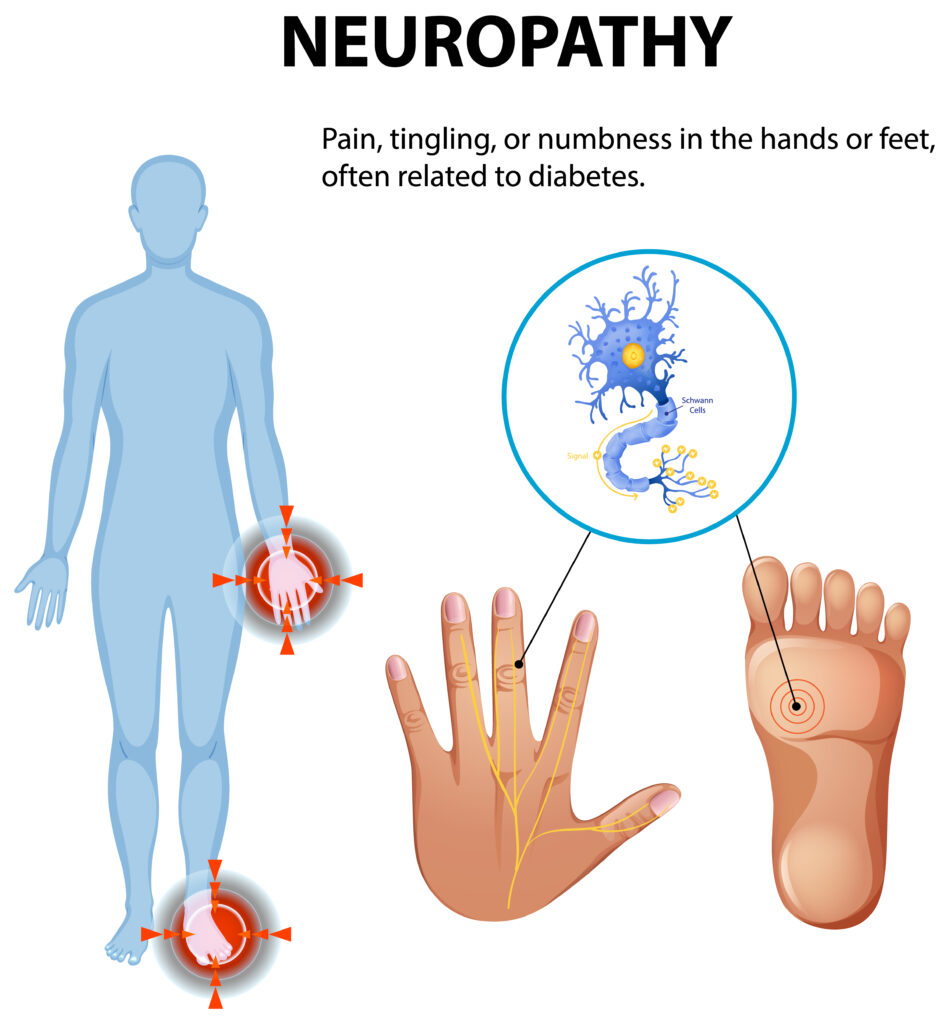
Early Warning Signs in the Diabetes and Neuropathy Relationship
In the early stages, the damage is subtle—a faint “pins and needles” sensation or a numbness in the toes that you might dismiss as fatigue. However, in the diabetes and neuropathy relationship, silence is dangerous. As metabolic strain continues, these sensations evolve into sharp, shooting pains or, more dangerously, a complete loss of feeling that can lead to unnoticed injuries.
Crucial Resource:
Managing weight and glucose is the first defense. If high costs are a barrier, exploring a cheaper alternative to Ozempic can help stabilize your readings before nerve damage becomes irreversible.
How High Sugar “Kills” Nerve Cells
According to Johns Hopkins Medicine, the mechanism is purely biological. When glucose levels redline, the body produces reactive oxygen species that damage cellular DNA. This isn’t just a “high reading”—it’s a chemical attack on your peripheral nervous system. Managing this relationship requires a dual-track strategy: controlling the sugar and supporting the nerves with neuro-protective compounds.
The Biological Impact of Glucose on Nerve Fibers
The diabetes and neuropathy relationship is fundamentally a story of starvation. In 2026, medical science has identified a state called “metabolic hypoxia.” Because sugar-induced inflammation constricts the tiny capillaries feeding your nerves, those nerves are essentially starved of oxygen. They stop firing correctly because they simply don’t have the energy to maintain their electrical charge.
Contextual Understanding:
The way nerve damage progresses can vary significantly depending on your diagnosis. Understanding the nuance between Type 1 vs Type 2 diabetes is crucial, as the autoimmune factors in Type 1 can sometimes present different neurological challenges than the metabolic resistance seen in Type 2.
Additionally, your lifestyle and genetics play a massive role. Identifying every diabetes risk factor—from sedentary behavior to sleep apnea—is the only way to build a comprehensive defense against neural decline.
To fix the nerves, you must first fix the flow. This is where understanding your glucose metabolism becomes non-negotiable. Without a stable metabolic foundation, your body’s natural repair mechanisms are overwhelmed. The protective myelin sheath, which acts like the insulation on a copper wire, begins to “short-circuit,” leading to the burning sensations many patients fear.
As noted by the National Institute of Health (NIH), nerve regeneration is possible, but only in a non-toxic environment. By optimizing how your body processes sugar and integrating neuro-protective nutrients that support the mitochondria (the power plants) of your cells, you can finally take a proactive stance against the diabetes and neuropathy relationship.
Common Questions About the Diabetes and Neuropathy Relationship
Is nerve damage from diabetes reversible in 2026?
While traditional views were pessimistic, the modern perspective focuses on “neural plasticity.” If you stabilize glucose and provide lipophilic nutrients that can cross the cell membrane, many patients report a significant reduction in pain and improved sensation over 6 to 12 months.
Why do my symptoms get worse at night?
This is a hallmark of the diabetes and neuropathy relationship. In the silence of the night, your brain has fewer external distractions, making it hyper-aware of the phantom signals from damaged nerves. Additionally, nighttime drops in core temperature can trigger “firing” in sensitive nerve endings.
Reclaiming your quality of life means looking beyond the blood sugar meter. It means understanding that your nerves are living tissues that require oxygen, stability, and nourishment. The diabetes and neuropathy relationship doesn’t have to be a one-way street toward disability—it can be the wake-up call that leads to your most disciplined and healthy era yet.
